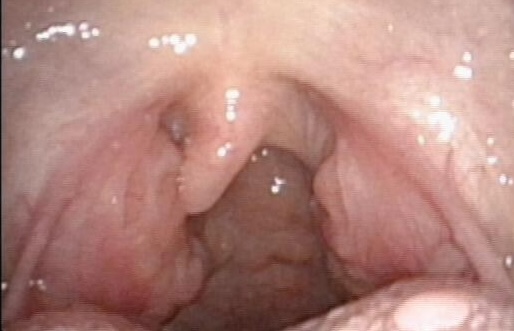
Does removing my child’s tonsils reduce their immunity?
1. Does Tonsil Removal Affect Immunity?
This is a common question that parents often pose. There is a prevalent view that tonsils are like sentries that protect the rest of the airway against infections
The evidence suggests otherwise. Tonsils are indeed part of the immune system — but their removal does not weaken immunity
The tonsils form part of the Waldeyer’s ring, a ring of lymphoid tissue that samples germs entering through the nose and mouth. However, by the age of 3, other immune tissues (lymph nodes, spleen, mucosal immunity) take over the same functions.
Studies show that children who have undergone tonsillectomy continue to produce normal levels of antibodies (IgA, IgG, IgM) and exhibit normal immune responses.
Conclusion: Removing tonsils does not cause immune deficiency.
2. Does tonsillectomy increase infection risk?
The evidence is mixed and must be interpreted carefully.
Short-term
In the months after surgery, some children get more viral upper respiratory infections, but this is temporary and reflects normal exposure at school rather than impaired immunity.
Long-term
Two types of studies exist:
A. Clinical ENT / paediatric studies (small-to-medium size)
These follow children for 1–5 years after tonsillectomy.
Findings:
- No increase in hospitalisations for infection
- No increase in serious infections
- No reduction in overall immune function
B. A single large Danish population study (Byars et al., JAMA Otolaryngology 2018)
This retrospective registry study (1.2 million children) reported:
- A small increase in relative risk of later respiratory infections in children who had tonsillectomy.
- But the absolute risk increase was extremely small, and the study had limitations:
- It did not account for why the tonsils were removed (children with more infections to begin with are more likely to be operated on).
- It combined minor infections (URTI) with major ones in its analysis.
- It did not examine intracapsular tonsillectomy, which preserves 10–20% of tonsillar tissue.
- Most ENT and paediatric societies concluded that this study does not change clinical practice, because:
- It is observational
- It is prone to confounding
- It contradicts decades of clinical evidence showing no immune harm
3. Intracapsular tonsillectomy preserves immune tissue
Modern coblation intracapsular techniques remove 80–90% of the tonsil but leave behind a thin rim of tissue.
Advantages:
- Lower bleeding risk
- Much less pain
- Faster recovery
- Preserves some lymphoid tissue, making any theoretical immune impact even less significant than with traditional tonsillectomy.
- There is no evidence that intracapsular tonsillectomy increases susceptibility to infections.
4. What do professional societies say?
American Academy of Pediatrics (AAP):
- Tonsillectomy does not result in impairment of a child’s immune system.
American Academy of Otolaryngology–Head & Neck Surgery (AAO-HNSF):
- Children who undergo tonsillectomy maintain normal immunologic function and do not have increased rates of serious infections.
ENT UK:
- The immune system fully compensates for the loss of the tonsils and adenoids.
Dr Jeeve Kanagalingam
Share this blog via: